When the body can't produce an adequate supply of hormones, it can cause health problems. This is where hormone replacement therapy plays an important role.
Hormone replacement therapy typically involves the use of synthetic thyroid hormones, such as levothyroxine, to restore the body's hormonal balance. In most cases, this effectively alleviates the symptoms of hypothyroidism and enhances the overall quality of life for affected individuals.
Before we delve deeper into how thyroid hormone replacement therapy treats acquired hypothyroidism, we should establish a background on what this condition actually is. Let's dive right in!
What is Acquired Hypothyroidism?
Acquired hypothyroidism, as the name suggests, refers to a thyroid disorder that develops later in life, distinct from congenital hypothyroidism, which presents from birth. At its core, hypothyroidism is characterized by an insufficient production of thyroid hormones within the body, leading to a cascade of adverse health effects.
In contrast, congenital hypothyroidism is diagnosed within the first couple of months of life. An infant with congenital hypothyroidism also has low levels of thyroid hormone but the causes are distinct from acquired hypothyroidism. Please click the link in this paragraph to learn more.
Causes of Acquired Hypothyroidism
Understanding the causes of acquired hypothyroidism is key to not only recognizing the condition but also to crafting effective treatment plans. Here, we delve into the primary factors contributing to this thyroid disorder:
Autoimmune Hypothyroidism (Hashimoto's Thyroiditis)
Hashimoto's thyroiditis, the most common cause of acquired hypothyroidism, is an autoimmune disorder. In this condition, the body's immune system erroneously identifies the thyroid gland as foreign and launches an attack against it.
Over time, this damages and eventually destroys the thyroid tissue, leading to a reduction in thyroid hormone production. The nature of Hashimoto's often means that symptoms develop gradually, making early diagnosis crucial for effective management.
Iodine Deficiency
Iodine, an essential mineral, plays a pivotal role in the synthesis of thyroid hormones. When the body lacks an adequate supply of iodine, it struggles to produce sufficient thyroid hormones.
This deficiency can be a result of a diet low in iodine-rich foods or living in regions where iodine is scarce in the environment. It underscores the importance of maintaining a balanced diet and, in some cases, taking iodine supplements to prevent iodine deficiency-related hypothyroidism.
Iatrogenic Causes
Iatrogenic hypothyroidism occurs as a consequence of medical treatments, often related to procedures or interventions involving the thyroid gland. These causes include:
- Thyroid Surgery or Radiation: Surgical removal of the thyroid gland, called thyroidectomy, or exposure to radiation therapy in the neck area can lead to hypothyroidism. These treatments are typically employed to address conditions like thyroid cancer or hyperthyroidism and lead to reduced thyroid function or hypothyroidism.
- Iodine-Containing Contrast Agents: Iodine-containing contrast agents, used in various medical imaging procedures, can temporarily affect thyroid function.
Who is at risk for developing acquired hypothyroidism?
Acquired hypothyroidism poses a risk to various individuals, particularly those with specific factors and conditions:
- Family History of Autoimmune Diseases: A genetic predisposition to autoimmune thyroid disorders increases the risk.
- Celiac Disease: Co-occurrence of celiac disease and hypothyroidism is more likely.
- Coexisting Autoimmune Conditions: Conditions like Type 1 Diabetes and Addison's disease elevate the risk due to shared autoimmune mechanisms.
- Gender Variation: Acquired hypothyroidism is more common in girls.
- Iodine-Deficient Diet: Relying solely on iodine-depleted sea salt can lead to iodine deficiency and, subsequently, hypothyroidism.
- Thyroid Cancer History: Previous thyroid cancer, requiring gland removal, may lead to acquired hypothyroidism and necessitate hormone replacement therapy.
- Iodinated Contrast Exposure: In children, iodinated contrast agent exposure during medical imaging can temporarily disrupt thyroid function.
Understanding these risk factors helps with early identification and personalized management of acquired hypothyroidism, emphasizing the importance of tailored healthcare for those at higher risk.
Symptoms of Hypothyroidism in Children
- Feeling tired
- Constipation
- Poor growth
- Weight gain
- Goiter or enlarged thyroid gland
- Dry skin
- Feeling cold
- Decreased metabolism
- Delays in puberty
- Abnormal lipid panel
- Muscle aches
- Delayed milestones
How is Hypothyroidism Diagnosed?
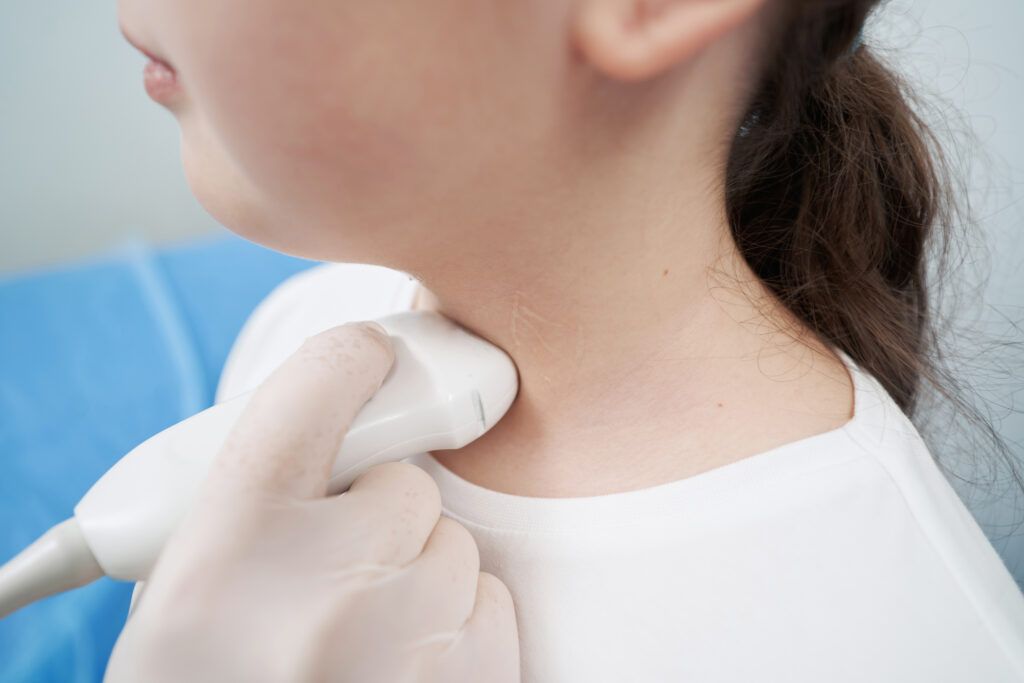
Diagnosing acquired hypothyroidism involves blood tests to measure TSH and T4 levels, along with clinical symptom evaluation and medical history assessment.
Once confirmed, treatment, typically involving thyroid hormone replacement therapy, is tailored to restore hormonal balance and alleviate symptoms. Early diagnosis and ongoing monitoring are essential to prevent complications.
How is it Treated?

Hormone replacement therapy is the cornerstone of treatment for acquired hypothyroidism. This therapy involves the administration of synthetic thyroid hormones, such as levothyroxine, to compensate for the inadequate hormone production by the thyroid gland.
By restoring normal hormone levels, this treatment alleviates the distressing symptoms of hypothyroidism, such as fatigue, weight gain, or growth failure. The therapy is precisely tailored to each patient's needs, emphasizing the importance of regular monitoring and dosage adjustments.
The Role of Levothyroxine (T4) in Hypothyroidism Treatment
The primary approach for addressing persistent or severe hypothyroidism hinges on thyroid hormone replacement therapy. This treatment involves the administration of levothyroxine or T4 in tablet form, and it is the most commonly prescribed therapy for hypothyroidism.
Remarkably, the majority of individuals with this condition experience substantial improvement in both their blood thyroid levels and the alleviation of their symptoms through this treatment. For instance, in the case of children facing growth issues due to insufficient thyroid hormone, growth rates typically rebound and normalize with the initiation of treatment.
Levothyroxine plays a vital role in restoring thyroid function and enhancing the overall well-being of those affected by hypothyroidism.
The Role of Liothyronine (LT3) in Thyroid Therapy
While LT3, or liothyronine, has been explored in the context of thyroid therapy, it has not demonstrated superiority over the conventional treatment with levothyroxine. This is because the human body converts T4 to T3, the biologically active form of thyroid hormone, which is usually sufficient for most individuals.
However, in cases where some continue to experience symptoms despite standard replacement therapy or have difficulty converting an adequate amount of T4 to T3, supplementation with liothyronine may be considered.
It's worth noting that research on this medication has primarily focused on adults, and its use in children is less common. Liothyronine can be administered in precise doses, distinguishing it from desiccated thyroid or thyroid extract, which is not recommended for pediatric use.
Results of Treatment
After starting thyroid hormone replacement therapy, routine lab monitoring typically occurs approximately 6-8 weeks from the start of treatment. However, there are specific situations where more frequent lab assessments might be recommended and based on individual needs.
This close monitoring is essential for fine-tuning the treatment plan and ensuring its effectiveness. Importantly, beyond the laboratory values, there may also be observable improvements in various symptoms associated with low thyroid levels.
These positive changes can manifest in enhanced energy levels, normalized growth parameters, or more favorable cholesterol levels. This provides further evidence of the treatment's effectiveness in optimizing thyroid function and overall well-being.
How to Live With Acquired Hypothyroidism

Once hypothyroidism is effectively treated, individuals can expect favorable outcomes. However, consistent adherence to prescribed medication is paramount.
It's advisable to establish a daily routine for taking medication, typically on an empty stomach, and separate from other medications or meals. Complementing medication management, maintaining a well-balanced diet, engaging in regular exercise, and ensuring restful sleep all contribute to healthier results.
Periodic lab evaluations are necessary and their frequency varies with age and also are guided by symptoms. Children and adolescents may require more frequent monitoring due to specific considerations.
Get Expert Advice from an Experienced Professional
If you or your child are at risk or exhibit symptoms of hypothyroidism, seeking expert evaluation and care from a board-certified Pediatric Endocrinologist is essential.

